Blog, News & Offers
Lets talk about Macular degeneration
Posted on Thursday, February 4, 2021

February is Low vision awareness month, Let's talk about Macular Degeneration
Macular degeneration is the most common cause of sight loss in people over the age of 50 in the UK. It is sometimes referred to as age-related macular degeneration or AMD or ARMD. There can be quite a bit of confusion cause about treatments for this condition especially from newspapers as there are 2 subtypes and the most common type has few treatment options.
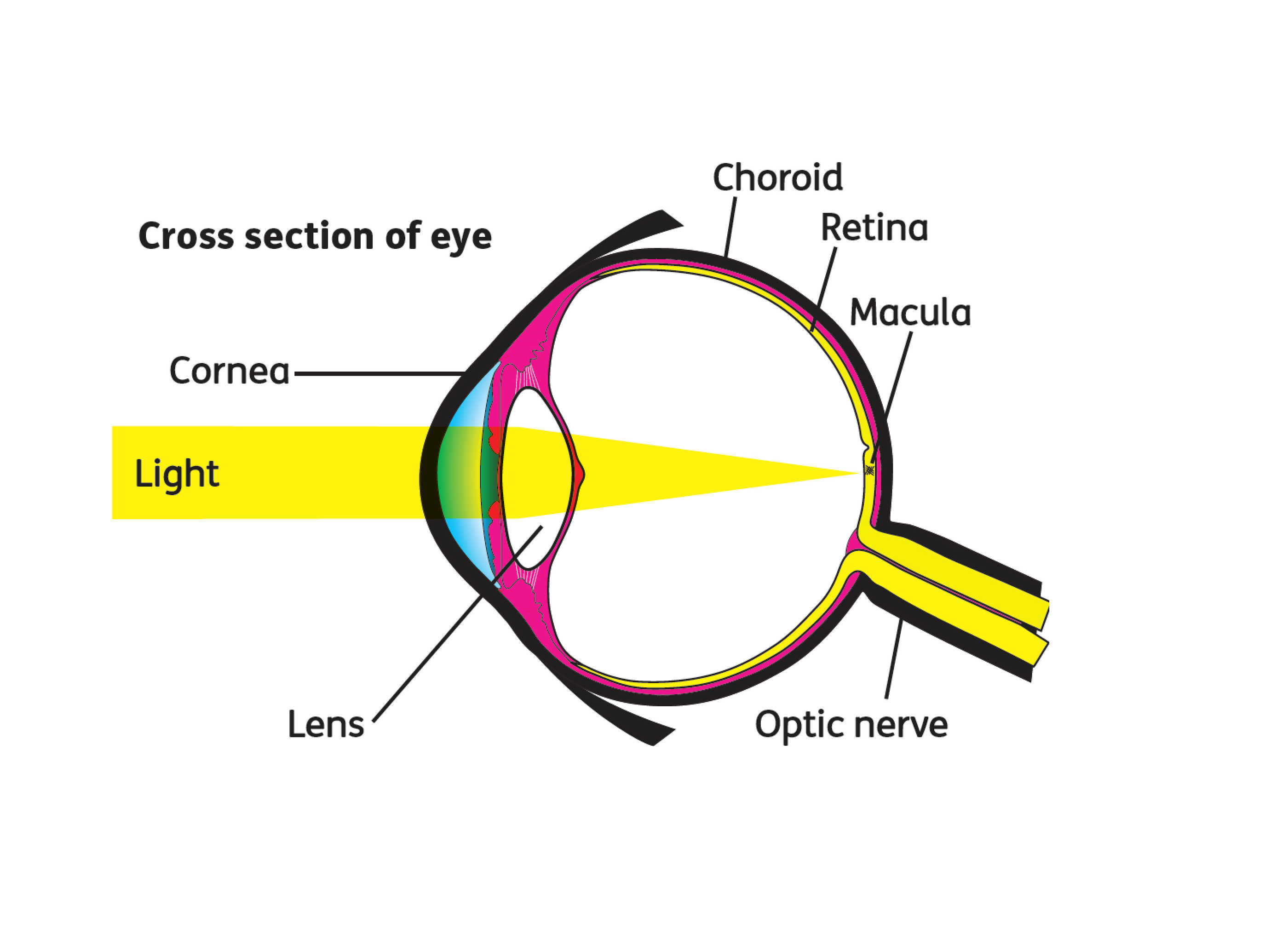
What is the macula?
The macula is part of the retina at the back of the eye. It is only about 5mm across but is responsible for our central vision, most of our colour vision and the fine detail of what we see. The macula has a very high concentration of photoreceptor cells – the cells that detect light. They send signals to the brain, which interprets them as images. The rest of the retina processes our peripheral, or side vision.
What causes AMD?
There are 2 types of macular degeneration Dry and Wet. Dry is the most common making up over 90% of cases.
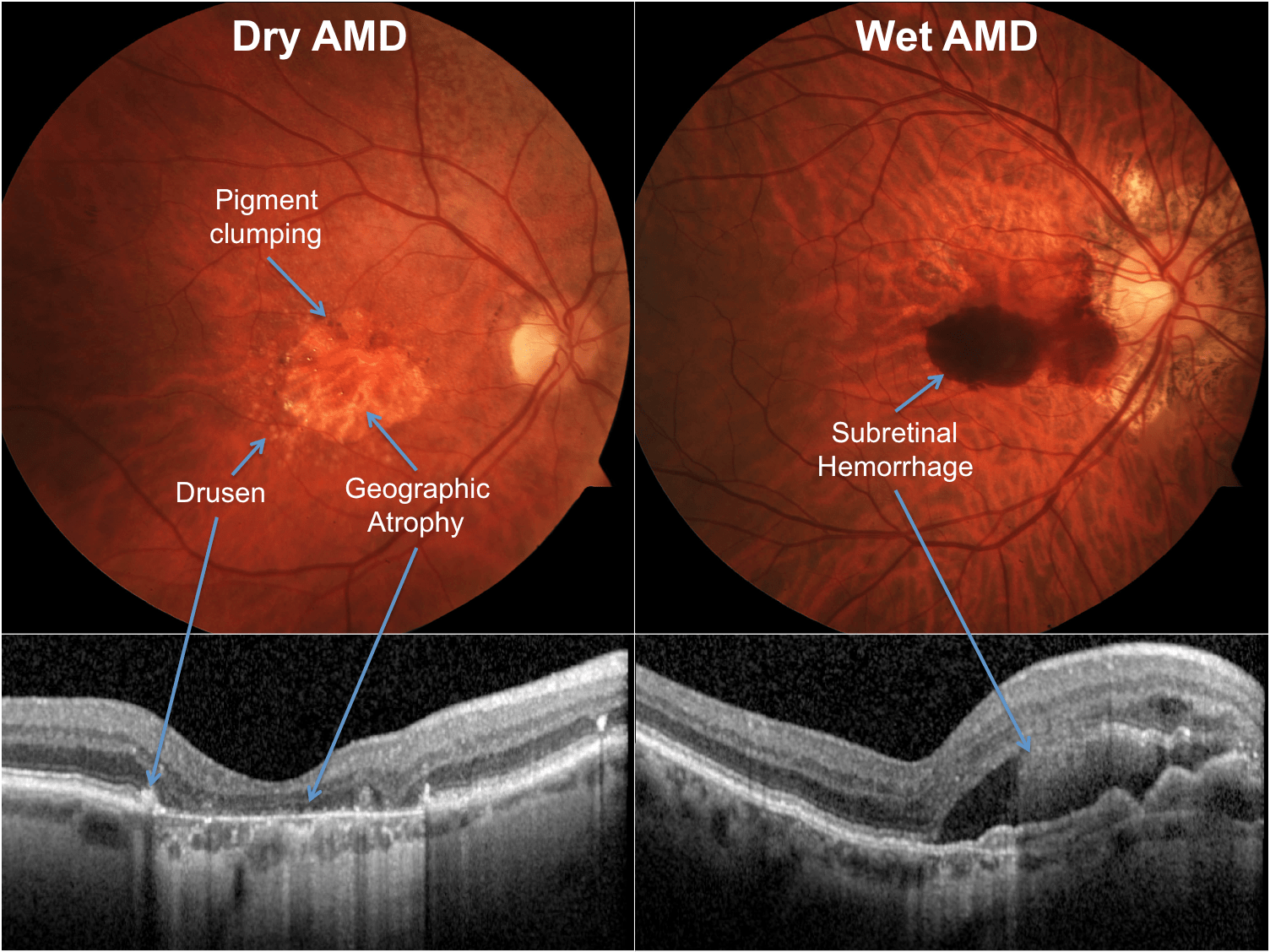
Dry AMD
Dry AMD is a slow deterioration of the cells of the macula, often over many years, as the retinal cells die off and are not renewed. The term ‘dry’ does not mean the person has dry eyes, just that the condition is not wet AMD.
The progression of dry AMD varies, but people often carry on as normal for some time.
Wet AMD
Wet age-related macular degeneration (AMD) develops when abnormal blood vessels grow into the macula. These vessels are weak and leak blood or fluid which leads to scarring of the macula and rapid loss of central vision. Wet AMD can develop very suddenly, but it can now be treated if caught quickly. Fast referral to a hospital specialist is essential.
A person with dry AMD can also develop wet AMD which is treatable, so it is important to act on changes in vision.
What are the symptoms?
The symptoms for both wet and dry AMD are similar although in wet AMD the symptoms occur quickly and are more severe with Dry occurring over a long period of time and going undetected or mistaken for general blurring of vision often assuming that a change in spectacles is needed.
The most commonly appreciated symptoms are:
• Gaps or dark spots (like a smudge on glasses) may appear in your vision, especially first thing in the morning. Objects in front of you might change shape, size or colour or seem to move or disappear.
• Colours can fade.
• You may find bright light glaring and uncomfortable or find it difficult to adapt when moving from dark to light environments.
• Words might disappear when you are reading.
• Straight lines such as door frames and lampposts may appear distorted or bent.
What causes AMD/risk factors?
• Age
• Family History of AMD
• Smoking
• Weight
• Exposure to UV (sun)
• High Blood pressure
Diagnosing AMD
AMD can be diagnosed by your Optometrist during routine or emergency sight testing.
In all sight tests we not only test for spectacle prescriptions but most importantly we look at the eyes health. There are parts of the eye which cannot be seen easily but the macular is positioned centrally so is a more easily assessed part of the eye. Sometimes however dilating eye drops are needed so that the bright light we use to view inside the eye stop your pupil from going small (the body’s normal, involuntary response to viewing bright lights)
As these changes often occur deep within the back of the eye viewing alone may not be enough to see changes occur and additional tests are needed such as OCT (Ocular coherence tomography) which can either be done at Hospital by referral or at some branches for an additional fee of £40.
OCT is also a good for providing your optometrist with a bench mark reading to look back on if changes in vision occur.
Treatment for AMD
There is no medical treatment for dry AMD, there are many research projects going on to find treatments or cures which you may read about in the news.
Several drugs are used to treat wet AMD. They are known as ‘anti-VEGF’ drugs. VEGF stands for ‘vascular endothelial growth factor’. It is the substance in the body that is responsible for the development of healthy blood vessels. In wet AMD, too much VEGF is produced in the eye, causing the growth of unwanted, unhealthy blood vessels.
Anti-VEGF drugs block the production of VEGF and stop the development of abnormal blood vessels. All the anti-VEGF drugs are given as an injection into the eye.
Lucentis® was the first anti-VEGF to be licensed for wet AMD. The normal procedure is that all patients receive a standard ‘loading dosage’ at the start of their treatment: normally three or more consecutive monthly injections. Eylea®.is another medication used but usually used for patients expected to be needing injections for longer as the interval between doses is increased and provided in non-consecutive months.
In December 2020, NICE (national institute of clinical excellence) announced that Beovu® had been approved to treat wet AMD. This new anti-VEGF treatment is longer-acting than the current treatments, and needs to be injected only around every 12 weeks. Patients who react well to the drug could have their injections spaced even further apart.
After this initial phase, there are a number of treatment regimens that an ophthalmologist can choose. Each regimen has a subtle difference in the frequency of appointments. They also vary as to whether or not you have an injection at every appointment.
Non medical treatments
Spectacles focus the light onto the macula as this is the most sensitive part of the eye, when damaged the peripheral vision becomes the most functional area of vision. Some people benefit from extra magnification for near as this makes the image falling on the back of the eye larger than the macular therefore falling on the functional part of the eye. Usually however people develop an enhanced use peripheral/eccentric fixation techniques, this technique requires someone to look away from or not directly at an object so it can be seen in their peripheral vision.
Hold out your hand and look straight at a finger, you can see the finger you are staring at in great detail. This is macula detail. While staring at the same finger notice the other fingers but do not look towards them, the detail isn’t as sharp but still functional. This is peripheral vision and falling on the retina.
There are now spectacles that force the image to fall onto a person’s best area of peripheral vision for them by looking straight ahead.
The peripheral area of the back of the eye is more sensitive to black and white vision rather than anything with colour. Yellow tints on spectacles can help to reduce colour perception and encourage black and white vision. For the same reason it is best that devices used around the house settings are adjusted to black and white mode like phones and televisions.
Making objects bigger can also help (magnification). Eg television; This can be done by moving televisions closer, investing in a bigger screen or by using low vision aids like magnifiers. The same principle applies to other objects.
There are many other low vision aids that can assist a person with sight loss for all manner of tasks such as whistles to alert you when pouring a cup of tea and stickers that can be applied to a cooker for finding popular heat settings. These can be purchased privately or available through low vision clinics.
An Ophthalmologist can refer patients to low vision clinics where expensive magnifiers and low vision aids can be loaned out to people after proper assessment to determine which powers or techniques will suit a person best.
There are also many support groups such as macular society as well as local support groups where people can share their experiences and assist people with suggestions.
Our dispensing opticians at every practice are trained in assisting patients learning eccentric or peripheral viewing techniques. The area which is best for each person is unique to them so must be found by trial and error. There are some things we can do with spectacles but we unfortunately will not be able to provide the improvements people desire from memory of corrected sight with glasses.
I hope this blog will be useful and if there is one takeaway point I would say is act quickly if you or someone you know mentions a loss in vision, swift action can lead to a better prognosis. We are open throughout the covid pandemic and beyond providing emergency and routine sight tests.
Blog Search
Blog Categories
- News (62)
- Sunglasses (3)
Blog Archives
- March2024 (1)
- November2023 (1)
- October2023 (1)
- August2023 (2)
- June2023 (2)
- April2023 (1)
- November2022 (1)
- October2022 (2)
- September2022 (1)
- August2022 (4)
- June2022 (3)
- May2022 (3)
- March2022 (3)
- December2021 (1)
- November2021 (2)
- July2021 (2)
- June2021 (1)
- May2021 (2)
- April2021 (3)
- March2021 (2)
- February2021 (4)
- January2021 (1)
- December2020 (1)
- November2020 (2)
- October2020 (1)
- September2020 (2)
- July2020 (1)
- April2020 (2)
- March2020 (3)
- January2020 (1)
- July2019 (3)
- June2019 (2)
- February2019 (1)
- October2016 (1)
- September2016 (1)
- June2016 (1)
Offices
- Aldridge (1)
- All Offices (24)
- None (37)